Flat a Hysterectomy May Not Protect Against Ovarian Cancer
Did you recognize it’s attainable to urge sex gland cancer even when you have had a hysterectomy? I learned the hard way. My sister, World Health Organization had a extirpation regarding ten years past, simply received a designation for a sort of sex gland cancer.
If you have got a partial extirpation, which removes your uterus, or a total hysterectomy, which removes your uterus and cervix, your ovaries remain intact and you can still develop ovarian cancer, according to the Mayo Clinic.
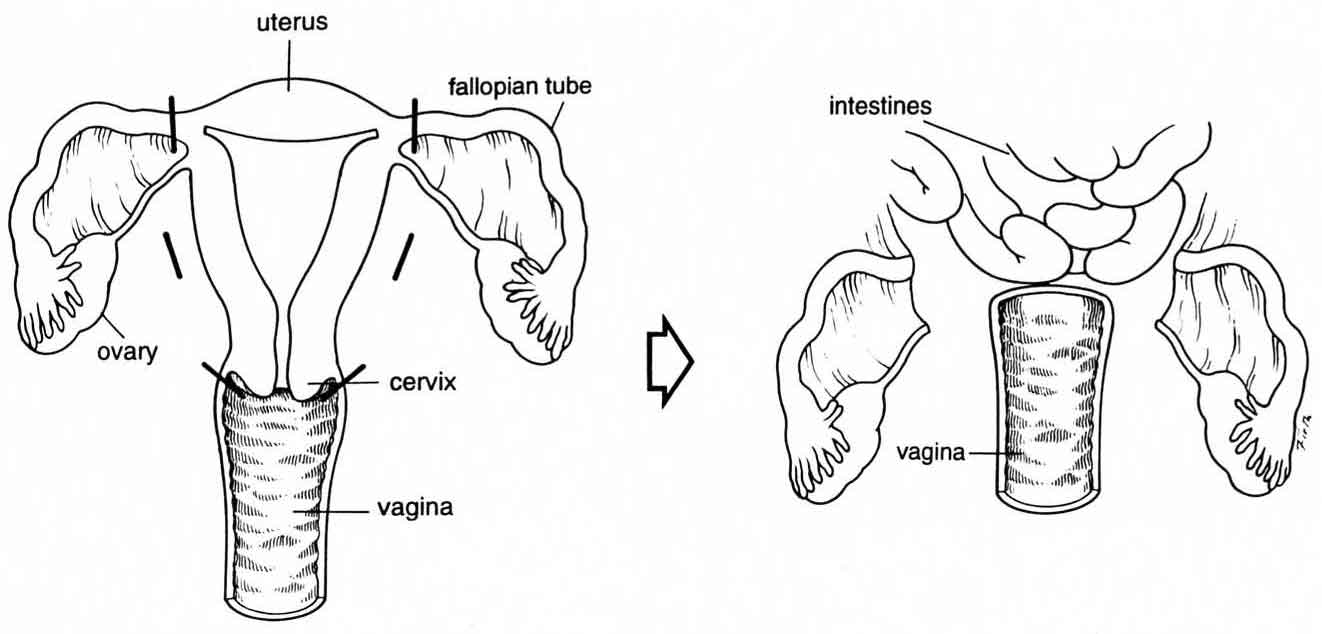
If, like my sister, you have a total hysterectomy with salpingo-oophorectomy, in which your cervix, uterus and both ovaries and fallopian tubes are removed, ovarian cancer is less likely but still can occur.
The details area unit confusing—surgeons speak quick and do not prefer to abate for patient explanations—but my sister’s doctor says she has primary liquid body substance malignant neoplastic disease, which looks and acts much like ovarian cancer and likely originated from ovarian cells.
As he explained it, when a woman undergoes a hysterectomy and has her ovaries removed, some ovarian tissue may be left behind. Ovaries are not well-formed organs like our liver or kidneys. They are soft tissues which will (and do) split up once you try and take away them. When items area unit left behind, some cancerous or precancerous cells may grow from that tissue. In some girls, the ovarian cells migrated to the peritoneal area during menstrual cycles before the ovaries were removed and became cancerous later on. It’s also troublesome to inform whether or not the cancer is coming back from sex gland or serous membrane cells—and it does not a lot of matter. It is treated the same.
My sister’s cancer appeared suddenly, without warning. Two weeks past, she started having severe abdominal pains. At first she thought it had been a abdomen virus or malady. But, after two days of worsening symptoms, her internist sent her to the emergency room. The ER doctor needed to send her home with a stool chemical, however my sister, being the strong-willed woman that she is, refused to leave.
When a doctor examined her consequent morning, he found a mass on her colon associate degreed set to try to to an emergencycolonoscopy. But, the mass was pressing down thus onerous on her colon that he could not do a endoscopy. The procedure suddenly became emergency removal of her entire colon because the mass had pinched off the tissue and killed it.
Once the doctor got within her abdomen, he discovered cancer cells throughout her abdomen. As he delineate them, they were sticky blobs of cells that were gluing her organs together. He removed what he might in what was changing into a drawn-out and sophisticated emergency surgery.
He wasn’t positive she’d pull through the surgery, but, thankfully, she did. We’re still obtaining answers and area unit a protracted means from winning the battle against cancer. But we’re extraordinarily glad that she’s lived to fight it.
I’ve learned a lot about ovarian cancer in the past week, and the most important thing I’ve learned is that it’s very important to get an early diagnosis—but there’s no screening take a look at for girls at average risk for sex gland cancer.
There area unit risk factors that may encourage your health care supplier (HCP) to be a lot of argus-eyed in searching for sex gland cancer, thus recognize your risk factors—and let your HCP recognize if you have any.
These are risk factors for ovarian cancer:
- A “first-degree” relative (mother, sister or daughter) who has or had ovarian, breast or gastrointestinal/colon cancer
- Age; most cases occur in women 60 and older
- Eastern European Jewish ethnicity (Ashkenazi)
- Mutation in the BRCA1 or BRCA2 gene
- Personal history of breast, endometrial/uterine or colorectal (colon) cancer
- Have never been pregnant or had trouble giving birth
- A high-fat diet
- Obesity
- Endometriosis
- Early start for your periods (before age 12) or later-than-average menopause (after age 50)
Of all risk factors, the foremost vital could be a case history of breast and/or sex gland cancer. However, it’s important to keep risk factors in perspective. Most women with risk factors for sex gland cancer can ne’er get sex gland cancer. And most ladies with sex gland cancer don’t have any robust risk factors for the illness.
The symptoms of sex gland cancer (particularly in its early stage) area unit typically not obvious or intense, however, if you have got better-known risk factors, you should definitely talk to your HCP if you notice any symptoms. Symptoms of ovarian cancer include:
- Pelvic or abdominal pain, pressure or discomfort
- Vague but persistent gastrointestinal upsets such as gas, nausea and indigestion
- Frequency and/or urgency of urination in absence of an infection
- Changes in bowel habits
- Weight gain or loss; particularly weight gain in the abdominal area
- Pelvic or abdominal swelling, bloating or a feeling of fullness
- Back or leg pain
- Pain during intercourse
- Vaginal bleeding or abnormal vaginal discharge
- Ongoing fatigue
If you or your HCP suspects you will have sex gland cancer, or you have a very high risk of developing it, you may undergo certain diagnostic tests, including imaging tests, biopsy and blood tests.
Your HCP could order a biopsy that checks for CA-125, a protein found in the blood of many women with ovarian cancer. However, alternative conditions, including normal ovulation, endometriosis and pelvic inflammatory disease can also raise CA-125 levels. And some girls with sex gland cancer could have traditional levels of CA-125. Because of these issues, the CA-125 test is not recommended for women at average risk of ovarian cancer.
Because my mother died of carcinoma and my sister currently has sex gland cancer, I know that I have significant risk factors. I will confer with my doctor regarding what testing is true on behalf of me. As with most cancers, early diagnosis is the key to survival.



