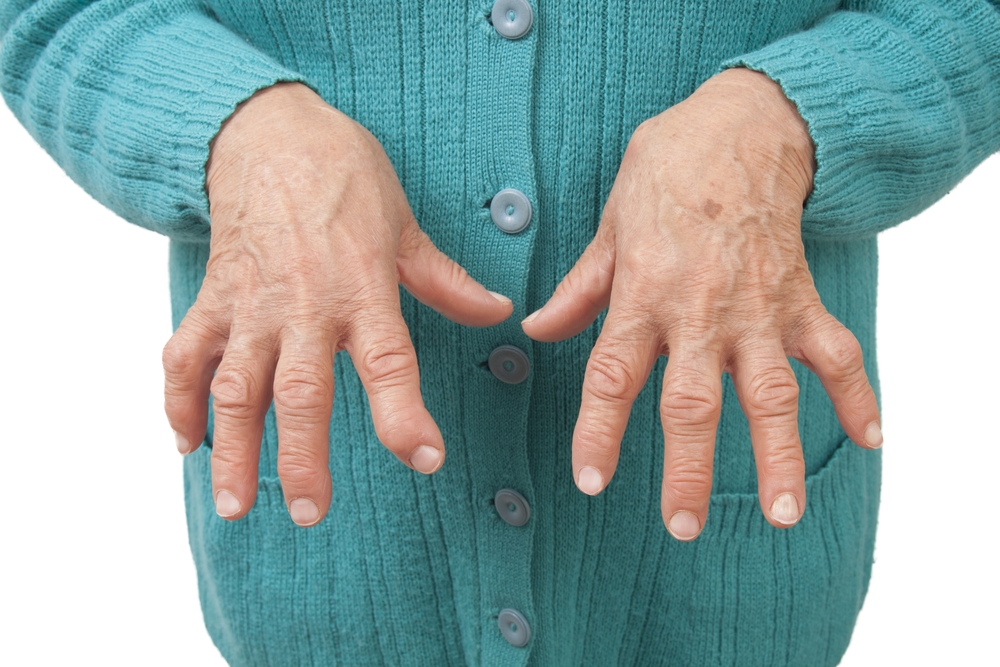
Why is rheumatoid arthritis (RA) sometimes called an autoimmune disease?
Overview
Rheumatoid arthritis (RA) is a chronic and potentially debilitating inflammatory disease that causes pain, swelling, stiffness and loss of function in the joints.
According to the Arthritis Foundation, RA affects about 1.3 million Americans, mostly women; two to three times more women have RA than men, and the number of women with the disease appears to be increasing. The age of onset can vary, but it typically occurs between ages 30 and 60, with the risk increasing as a person ages. The good news is that new advancements in treatment have made it possible to slow or stop the progression of RA.
Unlike the more common osteoarthritis, which is mainly a disease of the cartilage in joints, RA occurs when the body’s immune system attacks and damages the joints and, sometimes, other organs. RA often occurs in a symmetrical pattern, meaning that if one knee or hand is involved, the other one is, too.
The condition is considered an autoimmune disease. Such diseases area unit characterised by Associate in Nursing immune-system attack on the body’s healthy tissues. In RA, white blood cells travel to the synovium (the membranes that line the inner surface of the joint capsule) and cause inflammation, namely synovitis. The ensuing warmth, redness, swelling and pain are typical symptoms of RA, which usually affects the wrists, fingers, knees, feet and ankles.
The continuous inflammation associated with RA gradually destroys cartilage- the specialized tissue that coats and cushions the bony ends in the joints. The loss of cartilage leads to narrowing and loss of joint space and, eventually, damage to the bone. The surrounding muscles, ligaments and tendons that support and stabilize the joint also become weak and unable to work normally.
Systemic symptoms often include fatigue, general sense of malaise, low-grade fever, morning joint stiffness and difficulty moving a joint or several joints. Pain and signs of inflammation such as redness and warmth in or around a joint are often severe.
RA varies from person to person, but most cases are chronic, meaning they never go away. Some people have mild or moderate disease, with flares (periods of worsening symptoms) and remissions. For others, the disease is active most of the time. The resulting joint damage can be disabling.
The disease can affect more than just the joints, bones and surrounding muscle. About one-quarter of these with RA develop creaky nodules. These area unit bumps beneath the skin that always kind on the point of the joints. Many people with rheumatoid arthritis develop anemia. Other effects, which occur less often, include neck pain and dry eyes and mouth. Very rarely, RA results in inflammation of the blood vessels, the lining of the lungs, or the sac enclosing the heart. If you have RA, you may also be at increased risk for infections and gastrointestinal ailments.
Although no one knows the causes of rheumatoid arthritis, it seems to develop as a result of an interaction of several factors, including genetics, environment andhormones.
Diagnosing and treating rheumatoid arthritis can sometimes be difficult. It may require a team effort between you and several types of health care professionals, including arheumatologist, a physician who specializes in arthritis and other diseases of the joints, bones and muscles. Physical therapists, psychologists and social workers can also play a role.
RA can be devastating, but current treatment strategies can help you cope and possibly reduce the impact of the disease. These strategies can include pain relievers and other medications, rest, appropriate exercise, education and support programs. Involvement of the medicine health care skilled is crucial within the care of RA.
The psychological element is important: Some studies indicate that if you are well informed about your condition and participate in your own treatment plan, you will probably have less pain and create fewer visits to your health care skilled than otherwise. You can find treatment support groups in many cities.
Diagnosis
Rheumatoid arthritis (RA) can be difficult to diagnose in its initial stages, but an early diagnosis can be crucial to limiting its progress and severity. Some studies indicate that rheumatoid arthritis causes the most joint damage in the first two years.
There is no single test to determine if you have RA. The symptoms often are similar to those of other types of arthritis and joint conditions. The types of symptoms you experience—and the severity—may differ markedly from those of another person with RA. To make matters more confusing, symptoms can vary in the same person: Symptoms develop over time, and only a few may be present in the early stages of RA.
Often, RA is diagnosed by recognizing the type and pattern of joint involvement; it is a hallmark of RA, for example, if the same areas are affected symmetrically on both sides of the body.
The typical symptoms of RA include:
- tender, warm and swollen joints
- symmetrical pattern
- joint inflammation often affecting the wrists, fingers, knees, feet and ankles
- fatigue
- occasional fever
- a general sense of malaise
- pain and stiffness lasting for more than 30 minutes in the morning or after a long rest
- rheumatoid nodules (bumps under the skin—often formed close to the joints—that affect about a quarter of those with RA)
Less common symptoms can include neck pain and dry eyes and mouth. Very rarely, RA may cause inflammation of the blood vessels, the lining of the lungs or the sac enclosing the heart.
If you have any of these symptoms, you should visit a health care professional. He or she will take several factors into consideration before rendering a diagnosis:
- Medical history. Your description of the symptoms—including their duration and intensity—can help with the diagnosis.
- Physical examination. Your health care professional will do a physical exam and pay particular attention to your joints, skin, reflexes and muscle strength.
- Laboratory tests. Some laboratory tests will facilitate establish the presence of RA. Your health care skilled can most likely order a take a look at to notice autoantibody (an protein eventually gift within the blood of most of the people with unhealthy arthritis). It’s inconclusive, however, since not all people with RA test positive for rheumatoid factor, especially in the early stages. Some individuals with different sorts of rheumatic illness and alittle range of healthy people even have a positive autoantibody take a look at, so you could test positive and never develop the disease. A test called anti-cyclic citrullinated peptide, or anti-CCP, is now available and is more specific than rheumatoid factor tests. Specificity is even higher when both of the tests are positive. Other common tests include one that indicates the presence of inflammation in the body (the erythrocyte sedimentation rate, or ESR, and the C-reactive protein, or CRP), a test for antinuclear antibodies (antibodies that appear in about 30 percent to 40 percent of people with RA), a white blood cell count and a blood test for anemia.
- X-rays. These can help determine the extent of joint destruction. If you identify RA in its early stages, X-rays may not be helpful in diagnosis. However, they can be used to monitor the disease’s progress. Other imaging techniques, such as MRI and particularly joint ultrasound, have been shown to be very useful in assessment of the extent of inflammation and joint damage in RA.
Treatment
The main goals of rheumatoid arthritis (RA) treatment are to relieve symptoms of inflammation and to significantly slow the progression of joint damage. Although there’s no cure, you and your health care professional can develop strategies for keeping the disease under good control. You may need to try several approaches and different types of medication before you can satisfactorily relieve pain, reduce inflammation, slow joint damage and improve your ability to function.
In addition to the guidance of your primary health care professional, you may need care from a physical therapist, a rheumatologist (a physician who specializes in diagnosing and treating disorders that affect the joints, muscles, tendons, ligaments and bones) or an orthopedist.
When symptoms occur, you can take steps to lessen their severity. Protecting your joints from undue stress can help. Your health care professional can help you obtain a properly fitting splint. You may want to talk to him or her about self-help devices that can reduce stress on the joints while you participate in everyday activities. Zipper pullers, long-handled shoehorns and products that help you get on and off chairs, toilet seats and beds can all ease the strain on your joints.
Most likely, your treatment plan will include medications to relieve pain and/or reduce inflammation. Although there is no cure, disease-modifying antirheumatic drugs (DMARDs) may slow or stop the course of the disease. In the past, health care professionals often hesitated to prescribe these strong drugs until the disease had become relatively advanced. However, this approach has changed, especially for those who suffer from severe, rapidly progressing RA. Most rheumatologists believe that early treatment with additional powerful medication and therefore the use of drug combos is that the best thanks to halt RA’s progression and to scale back or stop joint harm. It is therefore important to establish care of RA with a rheumatologist as early as possible.
The following are commonly used rheumatoid arthritis medications:
- Analgesics. Analgesics are drugs that provide pain relief, and they can be used either orally or topically in people with RA. Analgesics include topical capsaicin (Capsagel), oral acetaminophen (Tylenol), tramadol (Ultram) and the more potent narcotics oxycodone (OxyContin) and hydrocodone (Vicodin). Narcotics are usually discouraged in the treatment of rheumatoid arthritis, however, because of the long-term nature of the condition and the danger of dependence.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs such as aspirin, ibuprofen, ketoprofen and naproxen help diminish pain, swelling and inflammation. However, each NSAID is a different chemical and can have different effects in the body.NSAIDs may cause side effects including ringing in your ears, bruising, heart problems, gastric ulcers, stomach irritation, and liver and kidney damage. The longer you use NSAIDs, the more likely you are to have side effects, and the more serious those effects can be. Many other drugs cannot be taken with NSAIDs—in particular, the blood thinner warfarin (Coumadin). NSAIDS should be used with caution in people over 65 and in those with any history of ulcers or gastrointestinal bleeding, congestive heart failure, renal insufficiency and hypertension. Even the nonprescription, over-the-counter forms of these medications have the same risks. It’s important to raise your health care skilled for safety info related to pain relievers together with your personal health history in mind.A newer NSAID (called a COX-2 specific inhibitor) inhibits an enzyme (COX-2), which triggers pain and inflammation, while sparing an enzyme called COX-1, which helps maintain the normal stomach lining. The COX-2 inhibitor celecoxib (Celebrex) is sometimes prescribed for RA, osteoarthritis and other pain-causing conditions, such as acute pain and menstrual cramps. Celebrex is presently the sole anti-inflammatory drug on the market. Celebrex might increase the chance of heart failure and stroke; discuss these risks together with your health care skilled. And if you’re presently taking Cox-2 inhibitor ANd suppose you’re having an hypersensitivity or produce other severe or uncommon symptoms whereas taking any nonsteroidal anti-inflammatory, decision your health care professional immediately. For more information on the risks associated with Celebrex.
- Disease-modifying antirheumatic drugs (DMARDs). These are slower-acting drugs, which work by altering the natural course of the disease and therefore slow or even prevent joint and cartilage destruction. They can produce significant results. You may need to wait weeks—even months—before seeing any effect, and you may use some or all of these, depending on the specifics of your condition. In some cases, one DMARD is used by itself. In other cases, more than one DMARD may be prescribed at the same time. You may have to try different medicines or combinations to find one that works best with the fewest side effects.Common DMARDs include: methotrexate (Rheumatrex, Trexall), sulfasalazine (Azulfidine), hydroxychloroquine (Plaquenil), leflunomide (Arava), cyclosporine (Sandimmune, Neoral), and azathioprine(Imuran, Azasan). People taking methotrexate and most other DMARDs need periodic monitoring to make sure that toxicity to the liver or bone marrow does not occur. Although there is clearly a potential for toxicity of a powerful drug like methotrexate, it actually has a remarkable safety profile in RA and can be taken continuously for many years. Side effects of DMARDS vary greatly but may include nausea or vomiting, diarrhea, heartburn, high blood pressure, sun sensitivity, rash, temporary hair loss, damage to the retina, liver or kidney damage, lung infections and bone marrow suppression.Pay attention to how your body responds to these drugs. Not only do you need to make sure the medications are effective (since efficacy can occasionally diminish over time), you also need to be alert to any problems arising from the drugs.
- Corticosteroids. Also known as glucocorticoids, corticosteroids such as prednisone and methylprednisolone (Medrol) reduce inflammation and pain and may slow joint damage from RA. Because they can cause dramatic improvements in a very short time, health care professionals often use them while waiting for DMARDs to kick in, and then may gradually discontinue use. They may be an option if your RA doesn’t respond to NSAIDs and DMARDs. These medications also have serious side effects, especially at high doses, including increased bruising, thinning of bones, increased appetite, weight gain, worsening of diabetes and cataracts.RA can increase bone loss, leading to osteoporosis. This bone loss is more likely in people who use corticosteroids for longer periods of time. To keep your bones as strong as possible, use the lowest possible dose of corticosteroids for the shortest amount of time, consume at least 1,000 to 1,200 milligrams of calcium and 400 to 1,000 IUs of vitamin D a day and talk to your doctor about medications called bisphosphonates, such as alendronate sodium (Fosamax) and ibandronate sodium (Boniva), that can help reduce bone loss.
- Biologic response modifiers. These are protein drugs that must be administered by subcutaneous injection or intravenous infusion. These drugs help to reduce joint-damaging inflammation by interfering with the inflammation process. The most commonly used short-acting drugs in this category are adalimumab (Humira), etanercept (Enbrel) and infliximab (Remicade). The longer-acting drugs in this category are certolizumab pegol (Cimzia) and golimumab (Simponi). They all target and inactivate a protein called tumor necrosis factor, or TNF-alpha, which is involved in the cascade of immune responses that cause inflammation in people with RA. Other biologic response modifiers target different molecules involved in the inflammation process. For instance, the drug anakinra (Kineret) blocks a cytokine called interleukin-1 (IL-1). Abatacept (Orencia) blocks the activation of T cells, and rituximab (Rituxan) blocks B lymphocytes. Tocilizumab (Actemra) is a biologic response modifier that inhibits interleukin-6. The biologic response modifiers are used as a second line drugs in individuals who do not respond to one or several TNF-alpha blocking agents.There have been very rare reports of serious nervous system disorders such as multiple sclerosis, seizures or inflammation of the nerves of the eyes, and serious infections, including sepsis and tuberculosis, with the TNF-inhibitors. The risk of tuberculosis has been greatly decreased with pre-therapy screening of TB skin tests and/or chest X-rays and treating with anti-TB drugs if these tests are positive.Additionally, there is some evidence that people treated with TNF inhibitors might have a somewhat higher risk of lymphomas. Although you need to be aware of these risks, it is equally important to recognize that the benefits can be substantial
- Non-biological DMARD. Recently, the U.S. Food and Drug Administration approved a new non-biological DMARD for RA treatment named tofacitinib (Xeljanz). This medication is the first in the new category of RA drugs that work by inhibiting intracellular enzymes called kinases. Tofacitinib is a JAK (Janus kinase) 1 and 3 inhibitor. Kinases are involved in generation of inflammation in RA. Tofacitinib has been approved as a second-line drug for RA patients who have inadequate response or are intolerant to a first- line DMARD methotrexate. Similarly to biologic response modifiers, Tofacitinib may increase risk for infection and cause liver abnormalities. In addition, in clinical trials, it has been associated with lipid and various blood cell count abnormalities in a small percentage of people. Your health professional will be able to tell if and when this new drug would be appropriate for treatment of your RA.
If you are taking a biologic response modifier and have an infection severe enough to require antibiotics, the biologic should not be given until the infection is gone.
If you are using DMARDs or biologics, you should not receive live-virus vaccinations. Discuss how to handle live-virus vaccinations with your health care provider.
Surgery could also be associate degree possibility if you’ve got severe joint harm. In the right circumstance, it can help reduce pain, improve the affected joint’s function and appearance and enhance your ability to perform daily activities. However, surgery is not right for everyone, and you and your health care professional need to discuss the best approach. Factors to consider include your overall health, the condition of the joint or tendon that will be operated on and cost of the surgery.
A common type of surgery prescribed for people with RA is joint replacement, which replaces your damaged joint with an artificial one. One thing to consider is that the artificial joints can wear out, necessitating additional surgery.
Tendon repair, most frequently performed on the hands, is a surgery that repairs overly loose or tight tendons around a joint.
In synovectomy, the inflamed synovial tissue is removed. Synovectomy is performed if the lining around your joint (synovium) is inflamed and causing pain, joint damage and loss of function that do not respond to conventional treatments.
RA may also require joint fusion (arthrodesis) or the surgical fusion of a joint to stabilize or realign it for pain relief in cases where joint replacement isn’t possible.
ClinicalTrials.gov, a service of the National Institute of Health, provides easy access to information on clinical trials for a wide range of diseases and conditions, including rheumatoid arthritis. The website is located.
What You Can Do to Combat RA Symptoms
While health care professionals must be involved in your care, there are a number of lifestyle changes you can make to help manage RA. Experts suggest that eating a healthy diet can enhance your overall health and thus help you better manage your RA. Although drinking has no known impact on the disease itself, you may need to avoid alcoholic beverages, depending on the RA medications you are taking, especially the often-prescribed methotrexate. Check with your health care professional. Stress reduction is also important, since your stress level may affect the amount of pain you feel.
Rest and exercise—seemingly opposite ends of the spectrum—are important to your health. When your RA is active, you will want more rest. But moderate exercise is critical to healthy muscles, joint mobility and flexibility. (Note: Discuss any exercise program with your health care professional before starting.)
While exercise may seem unappealing if you’re experiencing frequent pain, there are a number of techniques to help you get through a program:
- Moist heat equipped by heat towels, hot packs, a bath or a shower can be used at home for 15 to 20 minutes three times a day to relieve symptoms. Applying heat before exercise can be a good way to start. A health care professional can apply deep heat using short waves, microwaves and ultrasound to relieve pain.
- Cold equipped by a bag of ice or frozen vegetables wrapped during a towel helps stop pain and cut back swelling once used for ten to fifteen minutes. This treatment often is recommended for acutely inflamed joints. Do not use cold treatments if you have numbness or poor circulation.
- Hydrotherapy (water therapy) can decrease pain and stiffness. Exercising during a massive pool could also be easier as a result of water takes some weight off painful joints. Many community centers, YMCAs and YWCAs have water exercise classes developed for people with arthritis. You may also find relief from the heat and movement of a whirlpool.
- When performed by a trained professional, massage and manipulation (using the hands to restore normal movement to stiff joints) can help control pain and increase joint motion and muscle and tendon flexibility.
Although these forms of physiatrics will briefly relieve symptoms, none have documented anti-inflammatory effects or affect the rate of joint damage that can occur in RA.
Alternative Therapies for RA Pain Relief
- Relaxation techniques: Deep breathing, guided imagery and visualization (where you focus on “seeing” pleasant pain-free scenes or activities in your mind) and stress reduction help provide some pain relief. Physical therapists can teach relaxation techniques. The inflammatory disease Foundation includes a aid course that has relaxation therapy; establish a lot of regarding the inflammatory disease Foundation aid Program at
- Acupuncture: Acupuncture is an important component of traditional Chinese medicine that involves the insertion of thin needles at specific points, which are mostly along the body’s nerve pathways, to improve health. A handful of small studies have been conducted on the use of acupuncture in RA, and the findings do not clearly answer the question of whether or not it works. Individuals who want to use acupuncture should discuss their interest with their health care team. Only a licensed acupuncturist should be used.
- Thunder god vine: Studies indicate that preparations made from the peeled root of this plant, used in traditional Chinese medicine to treat inflammatory and autoimmune disorders, may be helpful in the treatment of RA. Possible side effects include menstrual changes, hair loss and diarrhea.
- Nutritional supplements: A few studies have shown that the nutritional supplement gamma-linolenic acid (GLA) and the fish oils eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) may help reduce some of the symptoms of RA.Discuss your interest or questions about such products and reports with your health care professional.
- Biofeedback: Biofeedback is a way to enhance an awareness of your body so that you become focused on how your body functions; usually this enhanced focus is turned toward something—such as muscle control—that usually happens at a subconscious level. During biofeedback, an electronic device provides information about a body function (such as heart rate) so you can learn to control that function. Biofeedback may help people with arthritis learn to relax their muscles. In this case, an electronic device amplifies the sound of a muscle contracting, so you know that the muscle is not relaxed. The therapy is typically learned with the help of a health care professional and then may be practiced at home once you have mastered the technique, either with a biofeedback machine or without one.
- Some additional techniques under investigation include tai chi (a movement- based form of meditation) and cognitive behavioral therapy (a method of anticipating and preparing yourself for situations and bodily sensations that will cause pain).
With all of these treatments—lifestyle, medical and surgical—monitoring which treatments work and which don’t and watching for side effects is critical. Monitoring can involve regular consultations with your health care professional as well as blood, urine and other laboratory tests and X-rays.
Prevention and Risk Reduction
Genetic, environmental and hormonal factors probably all play a role in the development of rheumatoid arthritis (RA). However, there is no known way to prevent RA. Cigarette smoking is one environmental risk factor for RA that you can avoid.
Certain genes involved in immune system responses are associated with a predisposition for developing RA, although there is no single “rheumatoid arthritis gene.” People with RA are more likely to have human leukocyte antigen (HLA) genes than people without the disease, and other genes also play roles in the development of RA. Having any of these genes is no guarantee that you’ll develop RA (in fact, many individuals with this common gene do not develop the disease); likewise, the absence of these genes doesn’t rule out the possibility of developing the disease. It appears that a person’s genetic make-up is an important part of the story, but not the whole answer.
Recent research shows that tobacco smoking can increase risk for RA. One study was conducted in Sweden and specifically looked at a population of more than 30,000 women. The study found significant association between development of RA and both smoking intensity and duration of smoking in women. The same study showed that such risk decreases over time, but it may take up to 15 years after smoking cessation to significantly reduce the risk. More and more studies seem to indicate that dental health is another important factor associated with RA. These are important advances in understanding the role of environmental factors in RA, because these factors can be avoided by not smoking and by flossing and brushing your teeth.
Facts to Know
- According to the Arthritis Foundation, rheumatoid arthritis affects approximately 1.3 million Americans, and two to three times more women have RA than men.
- RA is considered an autoimmune disease. Such diseases are characterized by the immune system attacking the body’s healthy tissues. Although RA affects other parts of the body, joint inflammation is the hallmark of this disease.
- Although no one knows the precise causes of rheumatoid arthritis, it seems to develop as a result of an interaction of several factors, including genetics, environmental factors and hormones. A virus or bacterium could serve as the environmental trigger in people genetically susceptible to the disease.
- Many researchers think a viral or bacterial infection may help trigger the development of RA. However, this remains unproven.
- Tobacco smoking may increase risk for developing RA.
- Rheumatoid arthritis appears to cause considerable joint damage in the first two years. An early diagnosis can be crucial in preventing the worst effects of the disease, especially since there are more effective treatment options today.
- Common RA symptoms can include fatigue, occasional fever, morning stiffness, difficulty moving a joint or several joints, pain and inflammation in or around a joint and a general sense of malaise.
- There is no single test you can take to find out if you have RA, although tests are used as part of the diagnosis.
- Arthritis literally means joint inflammation, but the term often is used to refer to more than 100 rheumatic diseases that can affect children and adults. Osteoarthritis is the most common form.
Key Q&A
- Why is rheumatoid arthritis (RA) sometimes called an autoimmune disease?Autoimmune diseases are characterized by an immune system attack on healthy tissues. In RA, white blood cells travel to the synovium (the membranes that surround joints) and cause inflammation, or synovitis. The ensuing warmth, redness, swelling and pain are typical symptoms of rheumatoid arthritis, which usually affects the wrists, fingers, knees, feet and ankles.
- What causes rheumatoid arthritis?A combination of factors—genetic, environmental and hormonal—probably plays a role in the onset of the disease. Those with a genetic susceptibility may develop RA when it is triggered by an environmental agent, perhaps a virus or bacterium, although no pathogenic agent has yet been identified. Hormones also appear to play a role. Tobacco smoking may increase risk for RA.
- Is RA preventable?No one has found a way to prevent RA.
- What can be done to reduce the pain or slow the disease?The symptoms of RA are highly treatable in most cases, and new research shows that the long-term outcome can be affected by how quickly the disease is diagnosed and treatment initiated. Consulting with your health care professional, you will find that there is a wide range of options—medical, surgical and lifestyle—available for modifying the disease and treating pain, swelling and other symptoms.
- How can I find out if I have RA?The symptoms you describe to a health care professional are the foundation of an RA diagnosis. The most common symptoms are tender, warm, swollen joints; symmetrical pattern of pain; joint inflammation; fatigue; occasional fever; a general sense of malaise; pain and stiffness lasting for more than 30 minutes in the morning or after a long rest; and rheumatoid nodules (bumps under the skin). Because many of these symptoms are also indicative of other diseases (for example, lupus), your health care professional may recommend lab tests for those diseases or for confirmation of an RA diagnosis, as well as X-rays and/or joint ultrasound to detect any joint damage. A full medical history and physical exam are also part of a typical diagnostic workup for RA.
- Is it safe to exercise if I have RA?Yes, moderate exercise is good for RA. However, you should consult with a health care professional before beginning any new exercise regimen and make sure that inflammation is reasonably well controlled. Moist heat applied before an exercise session and a cold pack applied afterward can help alleviate pain. Exercising in a swimming pool is also a good option for preventing joint stress during a workout.
- Can diet make a difference in preventing or managing RA?There is no scientific evidence that any specific food or nutrient helps or harms most people with rheumatoid arthritis. However, an overall nutritious diet with enough—but not an excess of—calories, protein and calcium is important. Some studies have shown that the omega-3 fatty acids in certain fish or plant seed oils also may reduce rheumatoid arthritis inflammation. However, many people are not able to tolerate the large amounts of oil necessary for any benefit, and both fish oils and plant oils have side effects, including risk of bleeding and interactions with certain medications, including blood pressure medications and psychiatric drugs. More research is necessary to find the optimal dosage of fish and plant seed oils for the management of RA.Some people may need to be careful about drinking alcoholic beverages because of the medications they take for rheumatoid arthritis. Those taking methotrexate may need to avoid alcohol altogether. You should ask your health care professional or a registered dietitian for guidance on the issue of diet.
- If I have the “RA gene,” does that mean I will develop the disease?There is no single RA gene. People with specific human leukocyte antigen (HLA) genes are more likely to develop RA than people without them, and other genes also play a role in the onset of disease. Having any of these genes is no guarantee that you’ll develop RA, and their absence doesn’t rule out the possibility of developing the disease. It appears that a person’s genetic makeup is an important part of the story but not the whole answer.



